Headaches are a common affliction that most people experience at some point. While they can range from a minor inconvenience to a debilitating condition, it’s crucial to understand the differences between various types of headaches and how to identify a migraine. Recognizing the common types of headache pain can help you manage your symptoms more effectively and seek the appropriate treatment when necessary.
Acute vs. Chronic Headaches
Before getting into specific types of headaches, it’s helpful to understand the difference between acute and chronic headaches. Acute headaches are typically short-lived and occur suddenly, often resolving within a few hours to a few days. They can be caused by factors like stress, dehydration, or illness. Chronic headaches, on the other hand, occur frequently and persist over a longer period, usually defined as 15 or more days per month for at least three months. Chronic headaches often require more extensive evaluation and management, as they can significantly impact daily life. Understanding the difference between acute and chronic headaches is crucial for effective treatment and prevention.
Primary vs. Secondary Headaches
Another important distinction to be aware of is primary vs. secondary headaches, which relate to the cause of a headache. Primary headaches are not caused by another underlying condition and include types like migraines, tension-type headaches, and cluster headaches. They arise from issues such as overactivity of pain-sensitive structures in the head. Secondary headaches; however, are symptoms of another medical condition, such as sinus infections, head injuries, or hypertension. The primary difference lies in their origin: primary headaches are standalone conditions, while secondary headaches are linked to other health issues. Proper diagnosis is essential to treat secondary headaches effectively, as addressing the underlying cause is crucial.
Common Types of Headache Pain
There are several common types of headaches, each with distinct characteristics and causes:
- Allergy or sinus headaches occur due to sinus inflammation and congestion often caused by allergies or infections. These headaches are typically felt in the forehead, cheeks, and bridge of the nose, and are often accompanied by other sinus symptoms like a runny nose, nasal congestion, and facial pressure or swelling. Treatment usually involves addressing the underlying sinus condition by using decongestants or antihistamines.
- Caffeine headaches are a frequent type of headache many people experience, often without realizing the cause. So, what is a caffeine headache? These headaches occur when a person consumes too much caffeine or suddenly reduces caffeine intake. What does a caffeine headache feel like? Typically, it manifests as a throbbing pain, similar to a tension headache, but it can also resemble a migraine with its intensity and duration. If you rely on caffeine and skip your usual dose, you might find yourself with a persistent headache. When it comes to how to get rid of a caffeine headache, managing your caffeine intake is key. Gradually reducing your caffeine consumption rather than quitting abruptly can help prevent these headaches, along with staying hydrated between your coffee breaks.
- Cluster headaches are less common but extremely painful. They occur in cyclical patterns or clusters, often waking people from sleep with intense pain around one eye or side of the head. These headaches can last for weeks or even months, followed by periods of remission. Cluster headaches are known for their sharp, burning, or piercing pain.
- Exertion headaches are triggered by physical activity, such as exercise, heavy lifting, or strenuous activity. They usually present as a throbbing pain on both sides of the head, lasting from a few minutes to a few hours. These headaches are more common in individuals who engage in high-intensity activities and can sometimes be prevented by proper warm-up routines and staying hydrated.
- Hemicrania continua, classified as a primary headache disorder, is a persistent headache that affects one side of the head. The pain is continuous without pain-free periods, can vary in intensity, and can last for days, months, or even years. It’s often associated with symptoms like tearing or redness in the eye on the affected side, nasal congestion, and drooping eyelids. Hemicrania continua is quite rare and typically responds to treatment with the medication indomethacin.
- Hormone headaches, or menstrual migraines, occur in relation to hormonal changes during the menstrual cycle. These migraines tend to be longer and more severe than regular headaches and often strike in the two or three days leading up to menstruation, continuing through to the first couple days of a period. Because this type of headache is associated with fluctuations in estrogen levels, its occurrence is more predictable than other types of headaches or migraines, which can strike at any time. Menstrual migraine can usually be treated the same way as other migraines. Tracking your cycle can also help you anticipate when you are most susceptible and help your health care provider develop the best treatment plan.
- Hypertension headaches are caused by high blood pressure. They typically present as a throbbing pain on both sides of the head and can come with symptoms like dizziness, blurred vision, or chest pain. These headaches are a sign that your blood pressure is dangerously high and require immediate medical attention to prevent serious complications such as stroke or heart attack. Hypertension headaches usually need to be treated with intravenous (IV) medication to lower your blood pressure gradually.
- Ice pick headaches, also known as primary stabbing headaches, are characterized by sudden, sharp, stabbing pains that typically last only a few seconds. They can occur several times a day and often affect the orbit (eye socket), temple, or parietal (around the top) area of the head. Despite their alarming nature, these headaches are usually benign and not associated with any serious underlying conditions.
- Post-traumatic headaches develop after a head injury or concussion. The pain can be similar to tension-type headaches or migraines, occurring days or even months after the injury. These headaches often require a multidisciplinary approach to treatment, including medications, physical therapy, and sometimes cognitive behavioral therapy to address the physical and psychological effects of the injury.
- Rebound headaches, also known as medication-overuse headaches, occur from the frequent use of headache medications. The headache returns as the medication wears off, leading to a cycle of medication use and headache recurrence. Reducing the use of headache medications gradually and under medical supervision can help alleviate rebound headaches and restore normal headache patterns.
- Spinal headaches, also known as post-dural puncture headaches, are caused by a cerebrospinal fluid leak through a puncture in the spinal cord’s membrane. This leak results in a drop in pressure around the brain and spinal cord. This type of headache can occur as a complication after a spinal tap or epidural anesthesia. They may also be caused by trauma or disease. Spinal headaches usually feel most intense when sitting or standing and improve when lying down. Treatment options include caffeine intake, bed rest, and, in severe cases, an epidural blood patch (a procedure where a small amount of a patient’s blood is injected into their lower back) to stop the leak.
- Tension-type headaches are among the most common types of headaches. They often feel like a constant ache or pressure around the head, particularly at the temples or back of the head and neck. Stress and muscle tension are typical triggers. While they can be uncomfortable, tension headaches are usually not severe and do not cause nausea or other symptoms typically associated with migraines.
- Thunderclap headaches are severe headaches that strike suddenly, like a clap of thunder. The pain peaks within 60 seconds and can last for hours. The headache intensity isn’t what differentiates thunderclap headaches from other headache types—it’s how fast the pain reaches peak intensity. The sudden, striking pain may be accompanied by fever, seizures, or an altered mental state. These headaches can be a symptom of a more serious condition, like bleeding in and around the brain, blood vessel damage, or a blood clot in the brain, and require immediate medical attention to rule out life-threatening causes.
Migraine vs. Headache Symptoms: How to Know When It’s a Migraine
Understanding the differences between a migraine vs. headache is essential for effective treatment. Migraines are a specific type of headache with distinct symptoms and often require different treatment approaches. Recognizing these symptoms is crucial in distinguishing migraines from other types of headaches.
Migraine symptoms can vary from person to person, but they typically include:
- Intense, throbbing pain on one side of the head.
- Nausea and vomiting.
- Sensitivity to light, sound, or smells.
- Visual disturbances, such as seeing flashing lights or blind spots.
So, how do you know if it’s a migraine? Pay attention to the specific symptoms and the severity of the pain. Migraines are usually more intense and debilitating than other types of headaches and are often accompanied by these other symptoms. Furthermore, migraines can last from a few hours to several days, whereas other headaches may not be as long-lasting.
If you struggle with headaches, and especially if you suspect you are experiencing migraines, it’s important to consult with a health care provider for an accurate diagnosis and appropriate treatment.
Managing Pain with gammaCore
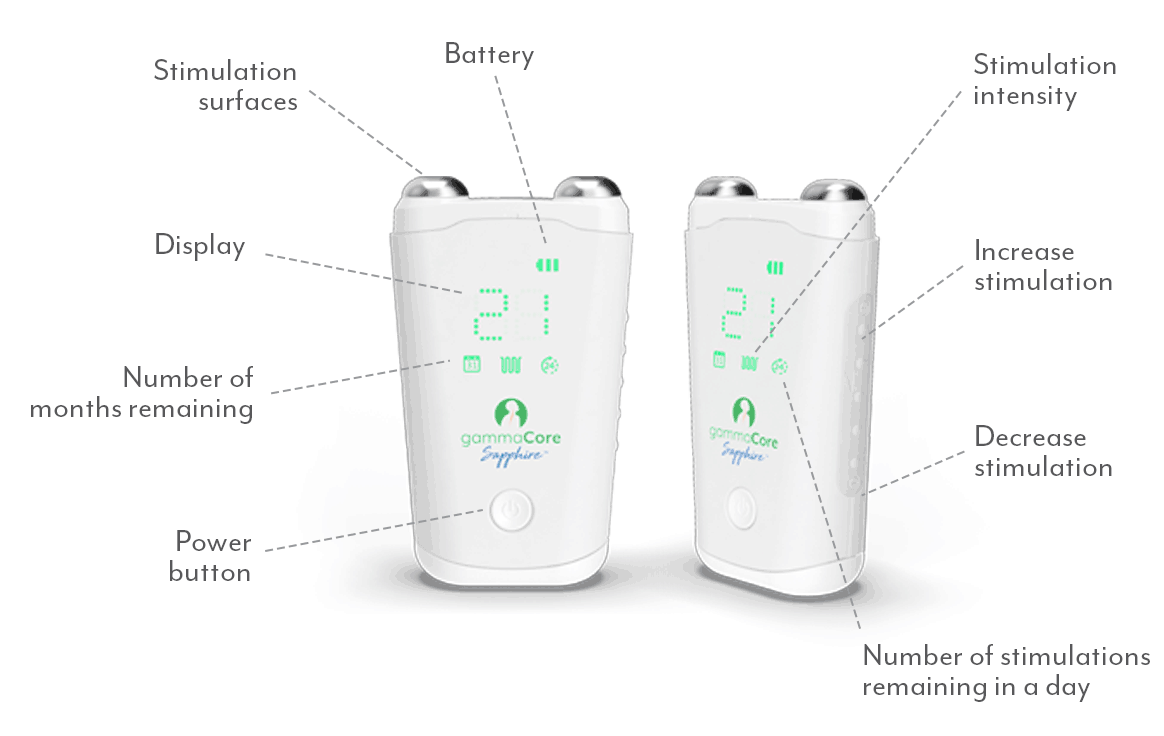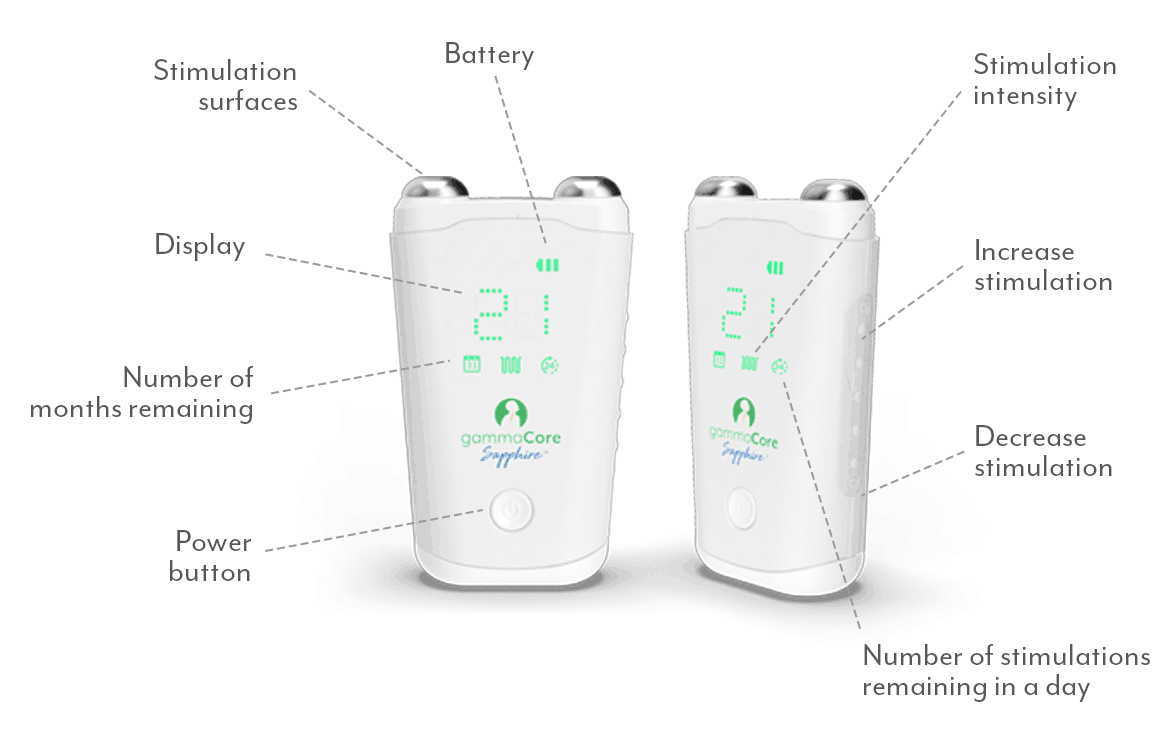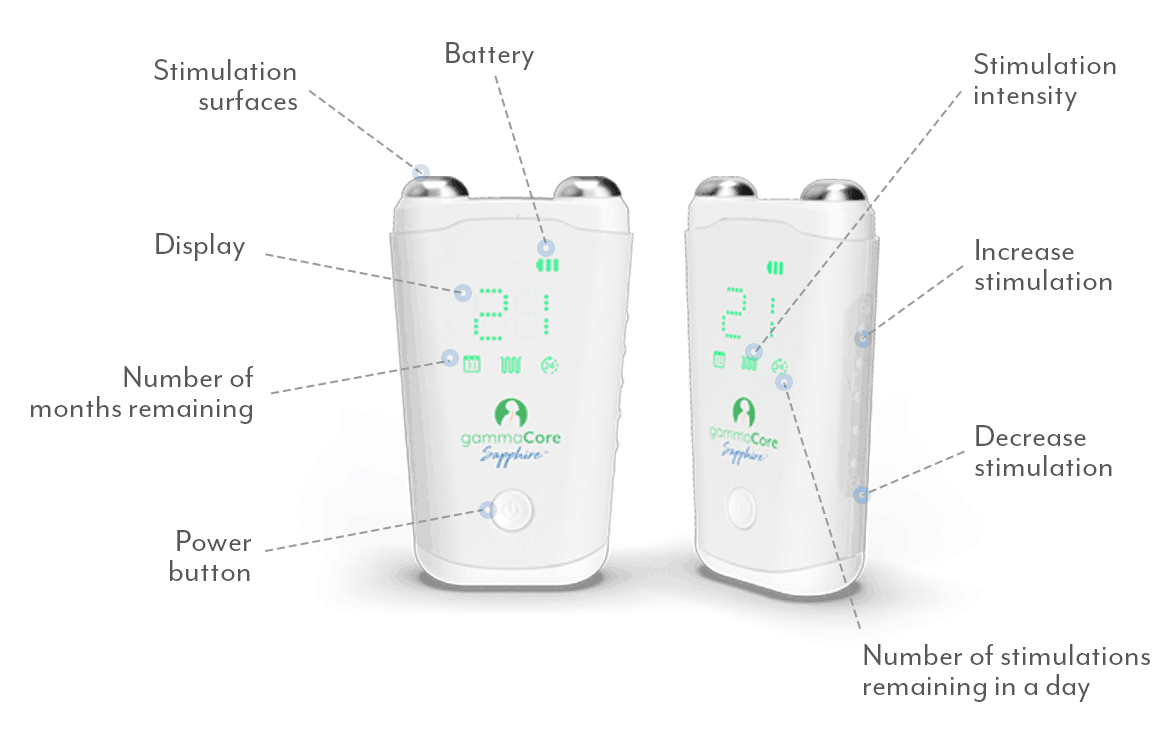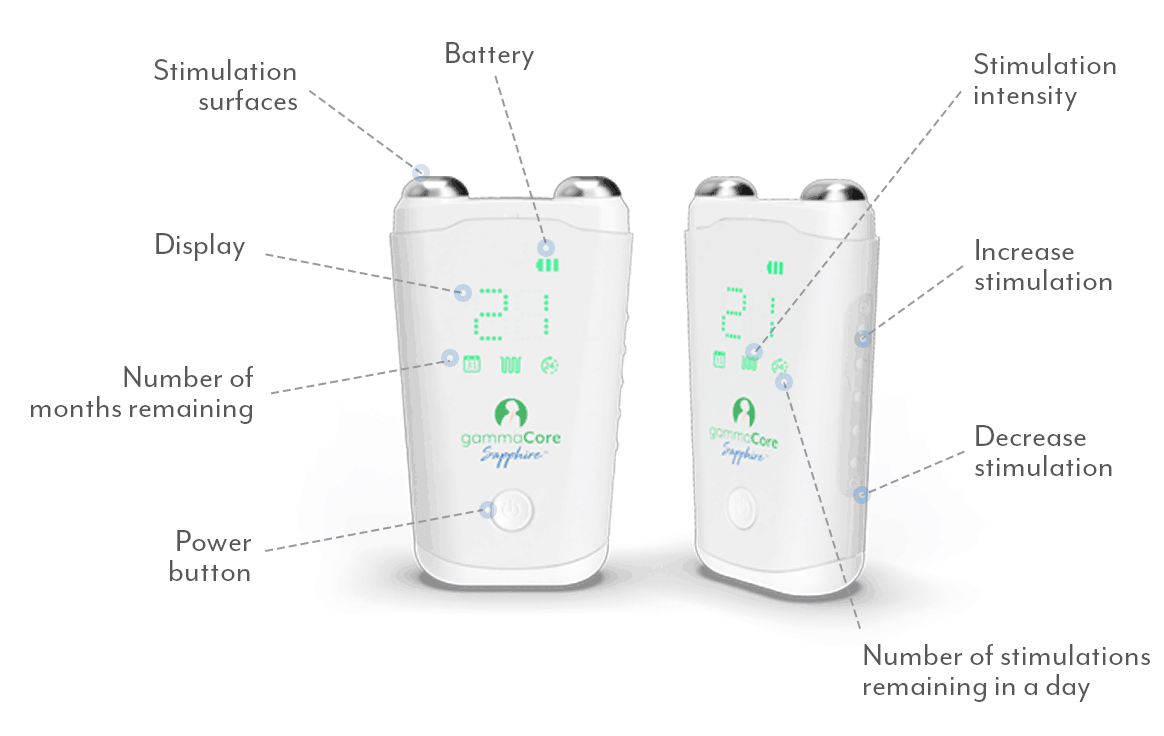
Whether you suffer from migraine or another type of headache, finding effective relief is essential. One innovative treatment option is gammaCore™ non-invasive vagus nerve stimulator (nVNS), a handheld, portable device with the broadest scope of headache indications for any prescription therapy, drug, or device.1
gammaCore nVNS is proven to provide relief and works by delivering gentle electrical stimulation to the vagus nerve, which can help alleviate migraine and headache symptoms and improve your quality of life.
To see if gammaCore is right for you, visit our clinic finder to help locate a health care provider near you, or contact our dedicated Customer Experience team at 888-903-2673 or customerservice@electrocore.com.
For important safety information and instructions for using gammaCore, please review the Important Safety Information and Instructions for Use.