The weather undoubtedly has a profound impact on our daily lives. Beyond affecting outdoor plans or wardrobe choices, it can also influence our health and well-being. For people prone to migraine, the connection between weather patterns and the onset of debilitating headaches is a well-known struggle. Weather-related migraines can cast a shadow over the sunniest days, but understanding the triggers and implementing proactive strategies can make a significant difference.
The Weather-Migraine Connection
Migraines are complex neurological events that often involve severe headaches, nausea, and sensitivity to light and sound. Weather-related migraines are triggered by changes in atmospheric conditions, including fluctuations in temperature, barometric pressure, humidity, and even stormy weather. Let’s break down how each of these factors can contribute to the onset of a migraine.
Barometric Pressure
Barometric pressure, or atmospheric pressure, is the weight of the air around us—it rises when the air is dry and drops when there’s moisture in the air. Changes in barometric pressure can be a significant trigger for migraines, often referred to as barometric pressure migraines or, more generally, barometric pressure headaches.1 Can barometric pressure cause headaches? Absolutely. As the pressure drops, typically before a storm, it can expand blood vessels in the brain, causing increased blood flow and triggering a migraine in susceptible individuals.2 This is why thunderstorms, with their rapid changes in atmospheric pressure, can be particularly challenging for migraine sufferers. Can storms cause headaches? Yes, the rapid shifts in pressure associated with storms can trigger migraines and other severe headache pain for some people. A change in barometric pressure can also create a pressure imbalance in the sinus cavity and within the inner ear, leading to severe headache pain for some people.3
Temperature
Extreme temperatures (hot or cold) and even sudden changes in temperature can trigger a migraine for some people. Some researchers believe that temperature impacts chemicals, like serotonin, in the brain—extreme or swinging temperatures can lead to an imbalance in these brain chemicals, which can lead to the onset of a migraine.4
Humidity
For some migraine sufferers, the amount of humidity in the air can have a significant impact on their headaches. One American study found there was a strong association between higher humidity levels and the onset of a migraine attack, as well as more intense headache pain.5 Hot, humid weather can also increase the likelihood of dehydration, a known migraine trigger.
Managing Weather-Related Migraine Pain
Understanding the weather-migraine connection is crucial for managing these headaches effectively. While you can’t control the weather, you can take proactive steps to minimize its impact. Here are a few practical tips to keep in mind.
- Monitor Weather Forecasts: Keep an eye on upcoming weather changes and plan accordingly. Knowing when to expect atmospheric shifts can help you take pre-emptive measures.
- Regulate Indoor Environment: Control temperature and humidity levels in your home to create a comfortable indoor environment. Use air purifiers and fans to circulate air effectively.
- Stay Hydrated: Drink lots of water throughout the day, especially during extreme weather conditions, to prevent a migraine triggered by dehydration.
- Control Other Triggers: You can control some migraine triggers, and focusing on these can help to reduce the impact of the weather. Maintain a regular sleep schedule, eat consistent meals throughout the day, manage stress levels, and avoid alcohol and typical food triggers.
- Medications: You can treat weather-related migraine pain with medications, as you would any other migraine. However, the one thing to remember is that weather can sometimes be unpredictable or last more than a day. Frequent use of acute medications may lead to medication overuse and make your headache symptoms worse in the long run.6
- Non-Drug Treatments: Several studies have shown that non-invasive vagus nerve stimulation (nVNS) is proven to be a safe and tolerable treatment method for preventing and treating migraine pain.7,8 Because it eliminates the need for pills or injections, you don’t have to worry about any drug-related side effects.
How to Treat Headaches from Weather Changes
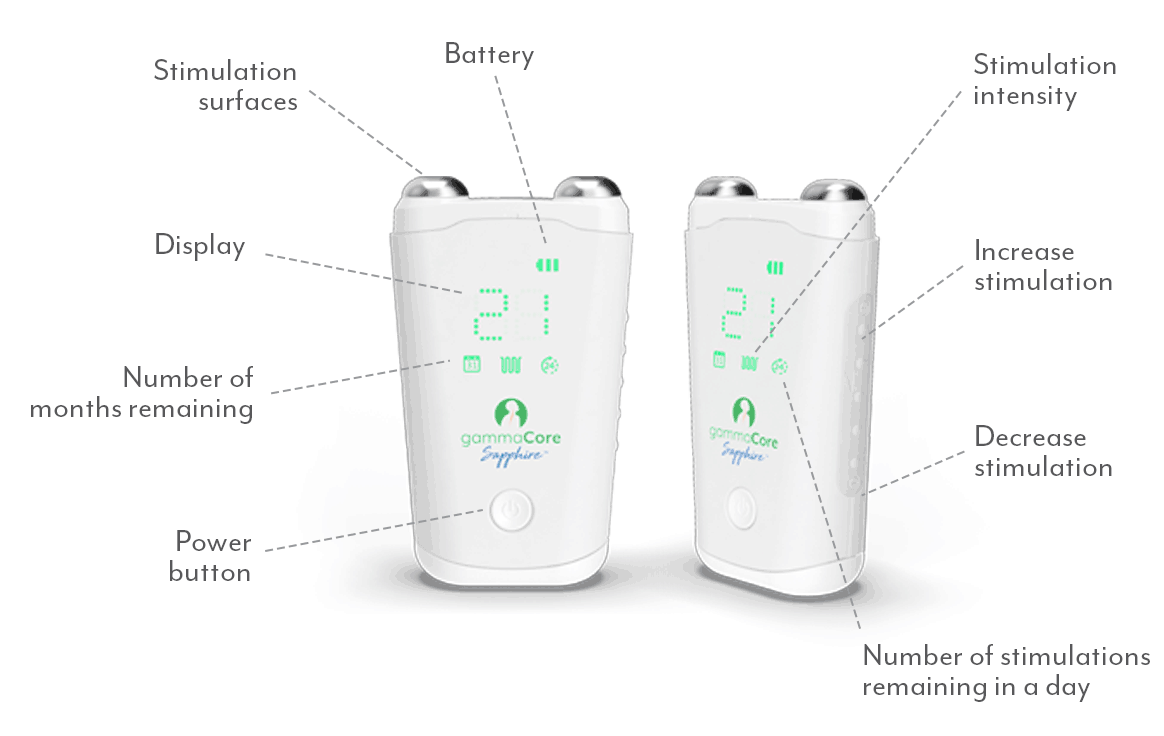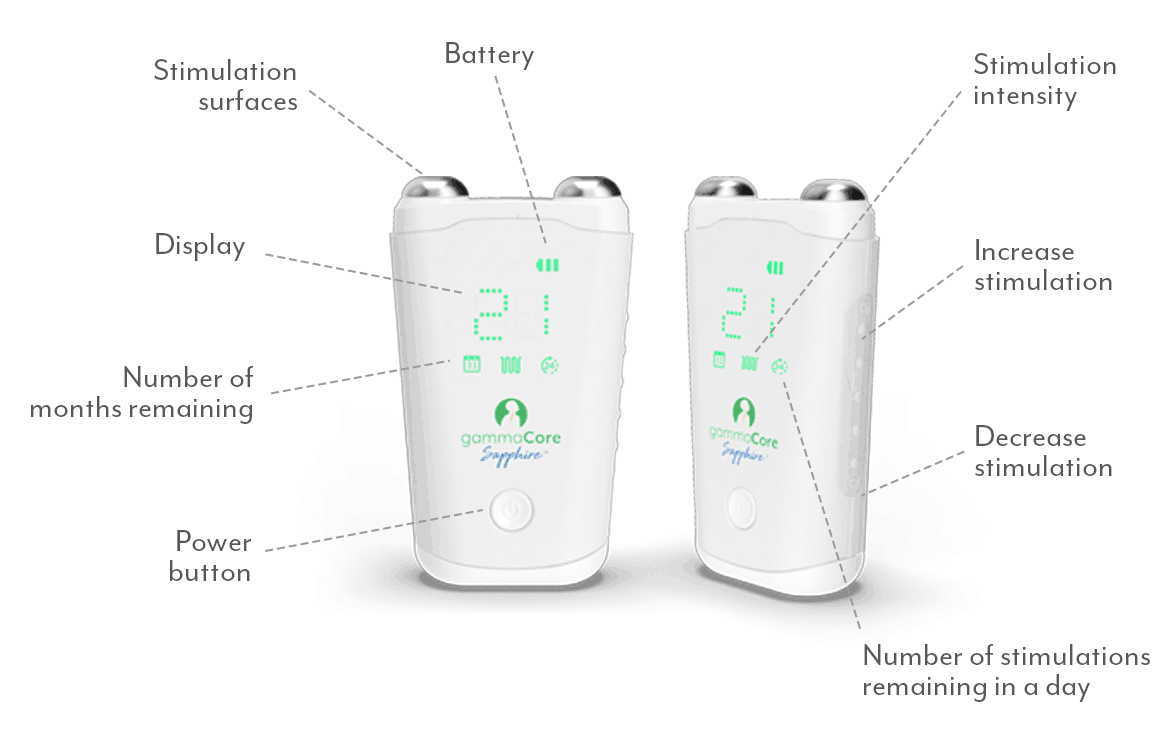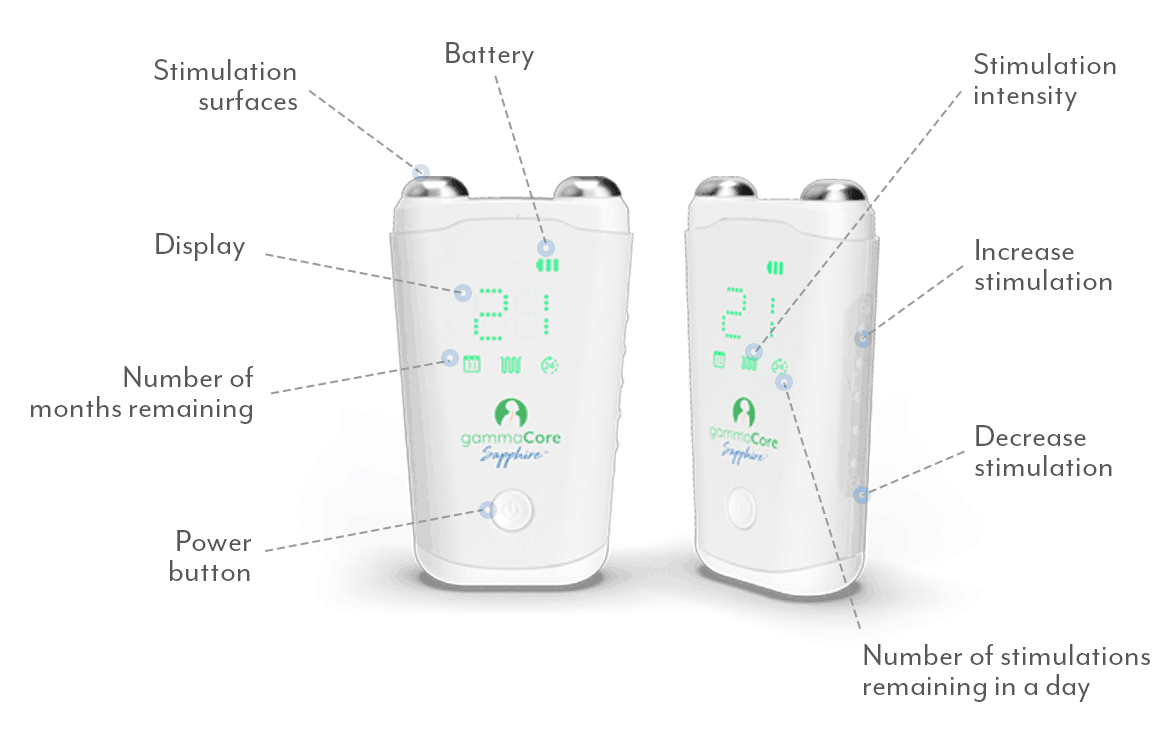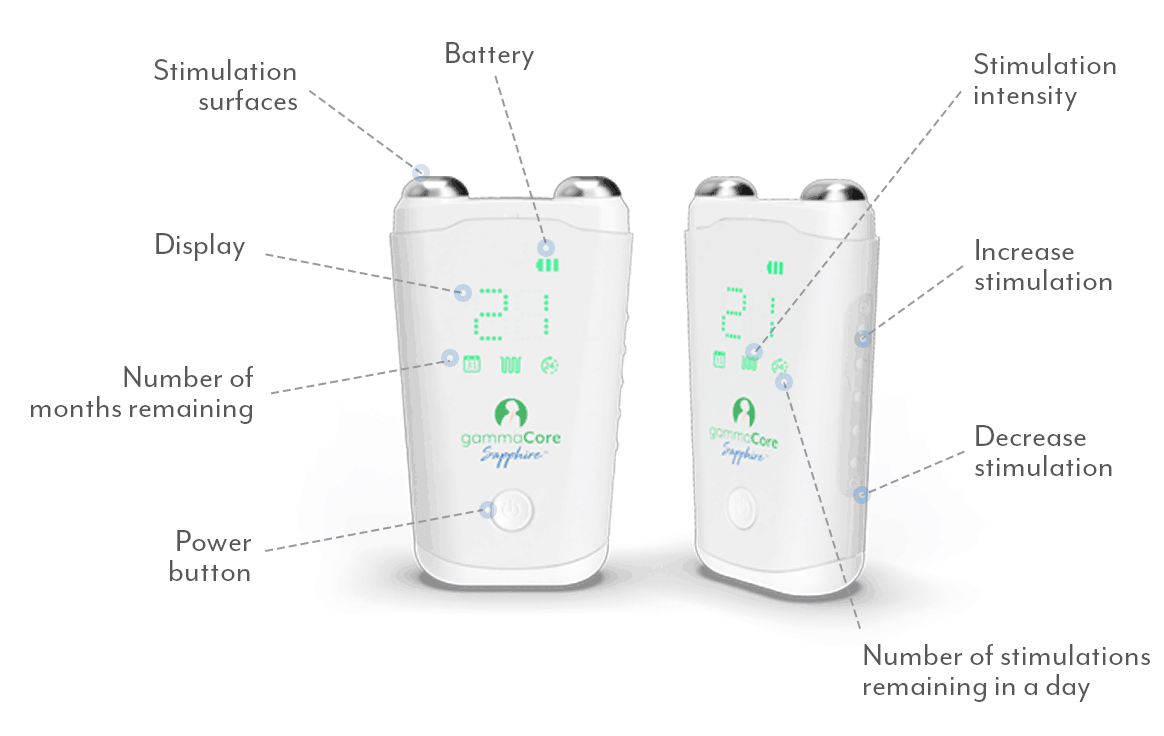
gammaCore non-invasive vagus nerve stimulator (nVNS) is the ideal solution for managing weather-related migraines because it can be used to both prevent future headaches and treat attacks when they strike, so you’ll always be covered. This small, handheld device works by non-invasively stimulating your vagus nerve, which blocks the pain signals in your brain that cause migraine attacks. It’s available by prescription from your health care provider, and treatments take less than 5 minutes—use it twice daily for prevention and up to 24 times a day for pain relief wherever and whenever you need it.
To see if gammaCore is right for you, visit our clinic finder to help locate a health care provider near you, or contact our dedicated Customer Experience team at 888-903-2673 or customerservice@electrocore.com.
For important safety information and instructions for using gammaCore, please review the Important Safety Information and Instructions for Use.
References
1. Kimoto, K., Aiba, S., Takashima, R., et al. (2011). Influence of barometric pressure in patients with migraine headache. Internal Medicine, 50(18), 1923-8. https://doi.org/10.2169/internalmedicine.50.5640
2. Okuma, H., Okuma, Y., & Kitagawa, Y. (2015). Examination of fluctuations in atmospheric pressure related to migraine. SpringerPlus. https://doi.org/10.1186/s40064-015-1592-4
3. Huizen, J. (2021, December 21). What you should know about barometric pressure and headaches. Medical News Today. Retrieved January 25, 2024, from https://www.medicalnewstoday.com/articles/320038
4. (n.d.). Are headaches triggered by weather changes? University Health Center by Nebraska Medicine. Retrieved January 25, 2024, from https://health.unl.edu/are-headaches-triggered-weather-changes
5. Hoffmann, J., Lo, H., Neeb, L., et al. (2011). Weather sensitivity in migraineurs. Journal of Neurology, 258(4), 596–602. https://doi.org/10.1007/s00415-010-5798-7
6. (2017, September 26). Spotlight On: Medication Overuse Headache. American Migraine Foundation. Retrieved January 26, 2024, from https://americanmigrainefoundation.org/resource-library/what-is-medication-overuse-headache/
7. Najib, U., Smith, T., Hindiyeh, N., et al. (2022). Non-invasive vagus nerve stimulation for prevention of migraine: The multicenter, randomized, double-blind, sham-controlled PREMIUM II trial. Cephalalgia, 42(7), 560-569. https://doi.org/10.1177/03331024211068813
8. Tassorelli, C., Grazzi, L., De Tommaso, M., et al. (2018). Noninvasive vagus nerve stimulation as acute therapy for migraine: The randomized PRESTO study. Neurology, 91(4). https://doi.org/10.1212/WNL.0000000000005857